Subscribe to the Newsletter
If you are interested in understanding how Traditional Chinese Medicine can improve your life sign up to my newsletter for the latest updates.
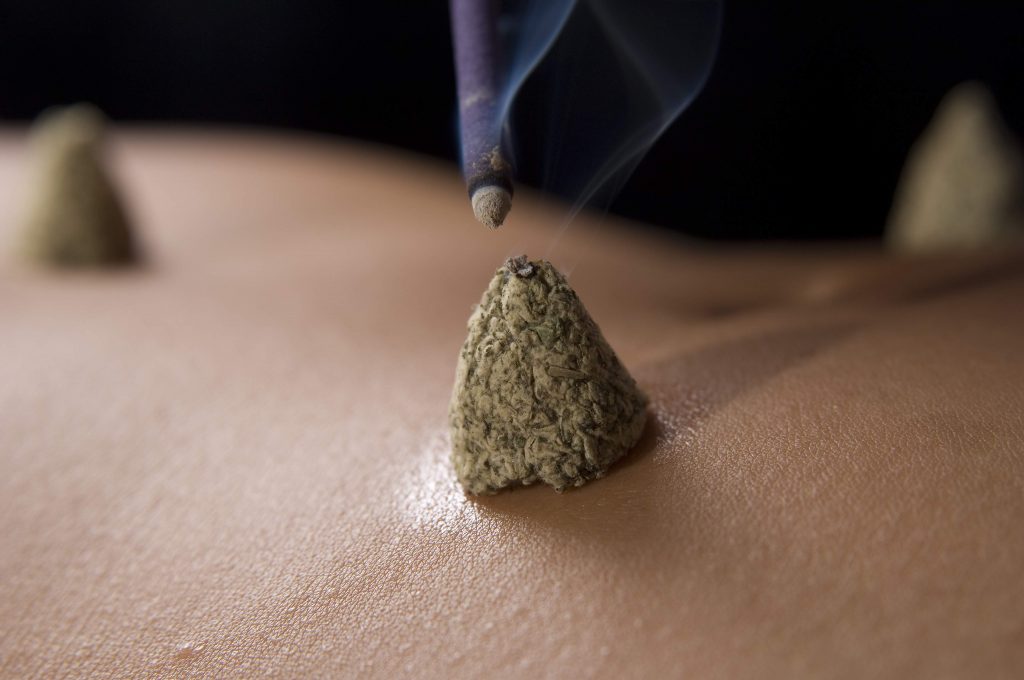
Interested in the results of research on moxibustion? (By the way, ‘moxa’ is short for moxibustion).
Moxibustion is an ancient form of treatment, mainly developed in China over the last three thousand years. It uses a pulverized herb, artemesia sinensis, which is burned over or on the skin or on inserted acupuncture needles.
People probably started using it in Northern China to combat the cold.
They almost certainly tried different substances over a long period, but the beauty of moxa is that it burns slowly, emitting a steady warmth, so is predictable in its effect.
As such, you can learn to use it safely.
It is, however, smelly, so modern Western-style hospitals and doctors don’t like it much!
And it burns, producing smoke and ash. Fire alarms don’t like that!
Read more about moxibustion here.
Here is some of what there is. We’ll add more in due course. So far there’s research on moxibustion for:
Moxibustion and acupuncture for the treatment of Crohn’s disease (Full Text World Journal of Gastroenterology, 08/29/2014 Clinical ArticleBao CH, et al).
In this randomized controlled trial, the authors aim to evaluate the clinical efficacy and safety of acupuncture and moxibustion for the treatment of active Crohn’s disease (CD). Moxibustion with acupuncture provided significant therapeutic benefits in patients with active CD beyond the placebo effect and is therefore an effective and safe treatment for active CD.
Ninety-two patients were equally and randomly divided into the treatment group and received herb-partitioned moxibustion combined with acupuncture, and the control group received wheat bran-partitioned moxibustion combined with superficial acupuncture.
The patients received three treatment sessions per week for 12 weeks and were followed up for 24 weeks.
The CDAI scores of both the treatment and control groups were significantly reduced after treatment compared with those measured before treatment.
However, the degree of improvement in the treatment group was significantly greater than that of the control group.
The improvement in symptoms in patients of the treatment group was sustained at follow-up, whereas that of the control group was not.
The overall efficacy of the treatment was significantly greater than that of the control.
Both groups demonstrated significant improvements in quality-of-life ratings after treatment. The improvement was significantly greater in the treatment group than in the control group.
In addition, the patients in the treatment group showed significantly increased HGB and significantly decreased CRP levels and histopathological scores at the end of treatment. In comparion, the control group did not exhibit significant changes.

Moxa has been used for thousands of years to help turn a baby when it’s the wrong way round in the womb before birth (breech presentation). What that means is that the baby’s bottom is facing the birth canal, not the baby’s head.
In the past, this usually meant that the baby would have to be surgically removed by opening the mother’s abdomen to remove the baby. Otherwise, since the baby’s bottom was too big for the birth canal, both mother and child would die.
This operation (Caesarean, after Julius Caesar who was apparently born that way) saved many lives. But of course it scarred the mother and still meant considerable danger for her, not least from sepsis.
I have treated many pregnant mothers with moxibustion to turn their babies. Here are results of some of the research on moxibustion that’s been done for breech presentation.
Cardini F. & Weixin H. (1998). JAMA 280(18), 1580-1584.
Abstract: Context.— Traditional Chinese medicine uses moxibustion (burning herbs to stimulate acupuncture points) of acupoint BL 67 (Zhiyin, located beside the outer corner of the fifth toenail), to promote version of fetuses in breech presentation. Its effect may be through increasing fetal activity. However, no randomized controlled trial has evaluated the efficacy of this therapy.
Objective.— To evaluate the efficacy and safety of moxibustion on acupoint BL 67 to increase fetal activity and correct breech presentation.
Design.— Randomized, controlled, open clinical trial.
Setting.— Outpatient departments of the Women’s Hospital of Jiangxi Province, Nanchang, and Jiujiang Women’s and Children’s Hospital in the People’s Republic of China.
Patients.— Primigravidas in the 33rd week of gestation with normal pregnancy and an ultrasound diagnosis of breech presentation.
Interventions.— The 130 subjects randomized to the intervention group received stimulation of acupoint BL 67 by moxa (Japanese term for Artemisia vulgaris) rolls for 7 days, with treatment for an additional 7 days if the fetus persisted in the breech presentation. The 130 subjects randomized to the control group received routine care but no interventions for breech presentation. Subjects with persistent breech presentation after 2 weeks of treatment could undergo external cephalic version anytime between 35 weeks’ gestation and delivery.
Main Outcome Measures.— Fetal movements counted by the mother during 1 hour each day for 1 week; number of cephalic presentations during the 35th week and at delivery.
The intervention group experienced a mean of 48.45 fetal movements vs 35.35 in the control group (P<.001; 95% confidence interval [CI] for difference, 10.56-15.60). During the 35th week of gestation, 98 (75.4%) of 130 fetuses in the intervention group were cephalic vs 62 (47.7%) of 130 fetuses in the control group (P<.001; relative risk [RR], 1.58; 95% CI, 1.29-1.94). Despite the fact that 24 subjects in the control group and 1 subject in the intervention group underwent external cephalic version, 98 (75.4%) of the 130 fetuses in the intervention group were cephalic at birth vs 81 (62.3%) of the 130 fetuses in the control group (P=.02; RR, 1.21; 95% CI, 1.02-1.43).
Conclusion.— Among primigravidas with breech presentation during the 33rd week of gestation, moxibustion for 1 to 2 weeks increased fetal activity during the treatment period and cephalic presentation after the treatment period and at delivery.
Free full text: http://jama.jamanetwork.com/article.aspx?articleid=188144
Coyle ME, Smith CA, & Peat B. 2012. Cochrane Database of Systematic Reviews 2012, Issue 5. Art. No: CD003928. https://www.cochrane.org/CD003928/PREG_cephalic-version-by-moxibustion-for-breech-presentation
Plain language summary
There is some evidence to suggest that moxibustion may be useful for turning babies from breech presentation (bottom first) to cephalic presentation (head first) for labour when used with either acupuncture or postural techniques of knee to chest or lifting buttocks while lying on the side.
Breech presentation of babies is common in the second trimester of pregnancy but most babies turn themselves before the onset of labour; some do not. A baby coming bottom first can have more difficulty being born, which causes trauma to the mother. A vaginal birth has to be planned or a caesarean section may be suggested. Moxibustion is a type of Chinese medicine that may be helpful in turning a breech baby. It involves burning a herb close to the skin at an acupuncture point on the little toe to produce a warming sensation.
This review found eight randomised controlled trials involving 1346 women. Women randomly assigned to moxibustion had daily to twice weekly treatment at between 28 and 37 weeks. In one trial adverse events relating to treatment included an unpleasant odour (with or without throat irritation), nausea and abdominal pain from contractions. The included trials were of moderate methodological quality, sample sizes in some of the studies were small, how the treatment was applied differed and reporting was limited. While the results were combined they should be interpreted with caution due to the differences in the included studies. More evidence is needed concerning the benefits and safety of moxibustion.
Vas J, Aranda-Regules JM, Modesto M, et al. (2013). http://www.ncbi.nlm.nih.gov/pubmed/23249535
Abstract OBJECTIVE: To compare the effectiveness of additional moxibustion at point BL67 with moxibustion at a non-specific acupuncture point and with usual care alone to correct non-vertex presentation.
This was a multicentre randomised controlled trial in which 406 low-risk pregnant women with a fetus in ultrasound breech presentation, with a gestational age of 33-35 weeks, were assigned to (1) true moxibustion at point BL67 plus usual care; (2) moxibustion at SP1, a non-specific acupuncture point (sham moxibustion) plus usual care; or (3) usual care alone. The primary outcome was cephalic presentation at birth. Women were recruited at health centres in primary healthcare.
In the true moxibustion group, 58.1% of the full-term presentations were cephalic compared with 43.4% in the sham moxibustion group (RR 1.34, 95% CI 1.05 to 1.70) and 44.8% of those in the usual care group (RR 1.29, 95% CI 1.02 to 1.64). The reduction in RR of the primary outcome in women allocated to the true moxibustion group compared with the usual care group was 29.7% (95% CI 3.1% to 55.2%) and the number needed to treat was 8 (95% CI 4 to 72). There were no severe adverse effects during the treatment.
Moxibustion at acupuncture point BL67 is effective and safe to correct non-vertex presentation when used between 33 and 35 weeks of gestation. We believe that moxibustion represents a treatment option that should be considered to achieve version of the non-vertex fetus.
Qin-hong Zhang, 1 Jin-huan Yue, 1 , 2 Ming Liu, 3 Zhong-ren Sun, 1 , 2 ,* Qi Sun, 1 , 2 Chao Han, 1 , 2 and Di Wang 1 , 2
Abstract: Objectives. This study aims to assess the effectiveness and safety of moxibustion for the correction of nonvertex presentation. Methods. Records without language restrictions were searched up to February 2013 for randomized controlled trials (RCTs) comparing moxibustion with other therapies in women with a singleton nonvertex presentation. Cochrane risk of bias criteria were used to assess the methodological quality of the trials.
Seven of 392 potentially relevant studies met the inclusion criteria. When moxibustion was compared with other interventions, a meta-analysis revealed a significant difference in favor of moxibustion on the correction of nonvertex presentation at delivery (risk ratio (RR) 1.29, 95% confidence interval (CI) 1.12 to 1.49, and I2 = 0). The same findings applied to the cephalic presentation after cessation of treatment (RR 1.36, 95% CI 1.08 to 1.71, and I2 = 80%). A subgroup analysis that excluded two trials with a high risk of bias also indicated favorable effects (RR 1.63, 95% CI 1.42 to 1.86, and I2 = 0%). With respect to safety, moxibustion resulted in decreased use of oxytocin.
Our systematic review and meta-analysis suggested that moxibustion may be an effective treatment for the correction of nonvertex presentation. Moreover, moxibustion might reduce the need for oxytocin.

While it is increasingly accepted that acupuncture for knee pain is effective, research on moxibustion for knee problems is as yet rare.
Yet moxibustion around the knee, when appropriate and according to the diagnosis in Chinese medicine, makes complete sense and is greatly appreciated by patients.
Here’s a study of research on moxibustion for the knee.
Ling Zhao1†, Ke Cheng12†, Lizhen Wang1, Fan Wu1, Haiping Deng1, Ming Tan34, Lixing Lao145 and Xueyong Shen12*
Our objective was to compare the effectiveness and safety of traditional Chinese moxibustion to that of sham moxibustion in patients with chronic knee osteoarthritis (KOA) pain.
We conducted a randomized placebo-controlled trial involving 110 patients with KOA who met the inclusion criteria. These patients randomly received either active moxibustion (n?=?55) or sham moxibustion control (n?=?55) at acupoints Dubi (ST 35), extra-point Neixiyan (EX-LE 4), and an Ashi (tender) point three times a week for 6 weeks. Effects were evaluated with Western Ontario and McMaster Universities’ Osteoarthritis Index (WOMAC VA 3.1) criteria at the end of the course of treatment and 3, 12, and 24 weeks after the initial treatment.
The WOMAC pain scores showed greater improvement in the active treatment group than in control at weeks 3 (P?=?0.012), 6 (P <0.001), 12 (P?=?0.002), and 24 (P?=?0.002) as did WOMAC physical function scores of the active treatment group at week 3 (P?=?0.002), 6 (P?=?0.015), and 12 (P <0.001) but not 24 (P?=?0.058). Patients and practitioners were blinded successfully, and no significant adverse effects were found during the trial.
A 6-week course of moxibustion seems to relieve pain effectively and improve function in patients with KOA for up to 18 weeks after the end of treatment. Moxibustion treatment appears to be safe, and the usefulness of the novel moxa device was validated.
Tuberculosis is a major source of ill-health and death, and becoming more common – again. Current medications are often no longer able to combat it. So it is essential that more work on possible ancient systems of medicine, such as research on moxibustion, be done.
Research on moxibustion for TB has been done by the Japanese and there’s a summary of some of the findings here:
Return from ‘research on moxibustion’ to our page on Moxibustion.

Stay in Touch!
No spam, only notifications about new articles and updates.

Book a Video consultation if you want to know more about your symptoms

This Introductory Chinese medicine course introduces you to the amazing thinking behind this ancient medicine, now increasingly in demand.

The Scottish College for Chinese medicine provides introductory courses for all, explaining Chinese medicine and its cultural background.

Master Tung’s acupuncture is a hidden treasure, lost to China but recovered in Taiwan from where it spread round the world.

Knee pain has five main causes. It’s certainly worth trying acupuncture before you resort to surgery!
Subscribe to the Newsletter
If you are interested in understanding how Traditional Chinese Medicine can improve your life sign up to my newsletter for the latest updates.
Subscribe to the Newsletter
If you are interested in understanding how Traditional Chinese Medicine can improve your life sign up to my newsletter for the latest updates.